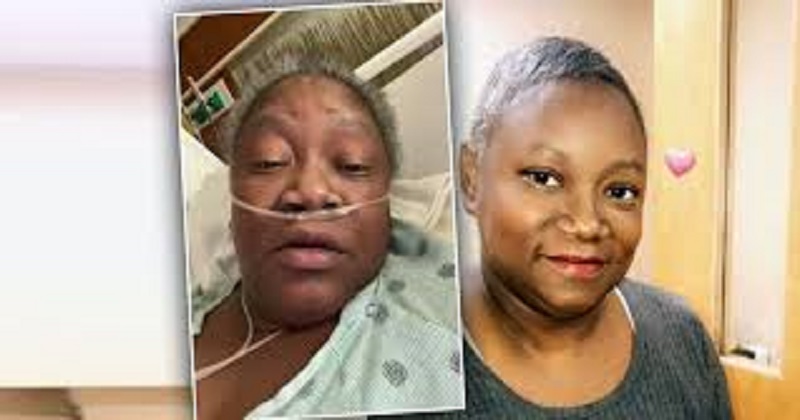
A black doctor in Indianapolis has lost his life with Covid-19 weeks after she blamed a doctor for refusing her proper medical supervision because of her ethnicity. In a video from her bed at Indiana University Hospital North, Susan Moore told that she had to “beg” for a cure. Delivering its condolences, the hospital said it took charges of racism very seriously but could not remark on distinctive patients. Black people are at greater risk from Covid than white people, studies show. Dr. Moore, 52, died at another local hospital on Sunday.
https://www.facebook.com/100003270157867/videos/3459156707536634/
On 4th December in her post on Facebook, she explained how her pain had been de-emphasized by the doctor, whom she said was white, though she had been screaming and having a problem with breathing.” He did not even listen to my lungs, he didn’t touch me in any way. He performed no physical exam. I told him you cannot tell me how I feel,” she wrote. A statement from the hospital said, “as an organization committed to equity and reducing racial disparities in healthcare, we take accusations of discrimination very seriously and investigate every allegation”.We stand by the commitment and expertise of our caregivers and the quality of care delivered to our patients every day.”
Dr. Moore is endured by her 19-year-old son, Henry, and her parents, who sorrow from dementia, according to a GoFundMe page formed up to assist obscure the family’s expenses. The page has already extended more than $102,000 (£75,000). Dr. Moore tested positive for Covid-19 on 29 November and was admitted with a high fever while she coughed up blood and toiled to breathe. But even as a physician herself, she said she had struggled with getting supervision.
Dr. Moore stated that she had had to beg for antiviral Remdesivir doses and request a scan of her chest. The doctor at one point told her she did not allow for the drug and that she should go home.”He made me feel like I was a drug addict,” Dr. Moore said in a Facebook video. “And he knew I was a physician. I don’t take narcotics. I was hurting.”Dr. Moore wrote she had asked a medical advocate and had requested to be moved elsewhere. She was finally discharged but had to return hours later after undergoing a drop in blood pressure and fever.”This is how black people get killed,” Dr. Moore said. “When you send them home and they don’t know how to fight for themselves.”
Her post later contained an update stating the hospital’s chief medical officer had said staff would obtain diversity practice. But a promise for an apology from the doctor she blamed of racism fell through.” I put forward and I maintain, if I was white, I wouldn’t have to go through that,” she said. Dr.Moore’s experience and death have flared an uproar over US healthcare discrepancies encountered by black Americans.
The virus has disproportionately impacted black and other minority communities in the US. Black Americans are three times more likely to die from the virus than white Americans. An estimation by the Brookings Institution conveyed “in every age category, black people are dying from Covid at approximately the same rate as white people more than a decade older”.

Post Your Comments